Hearing Loss and Vision Disturbances: Clinical Perspectives
Sensory changes like hearing loss and vision disturbances can arise from various underlying conditions, including neurological disorders. While these symptoms are often linked to age-related decline or localized issues, they may occasionally signal more serious health concerns. Understanding the relationship between sensory impairments and potential neurological conditions helps individuals recognize when medical evaluation is necessary and supports early intervention strategies.
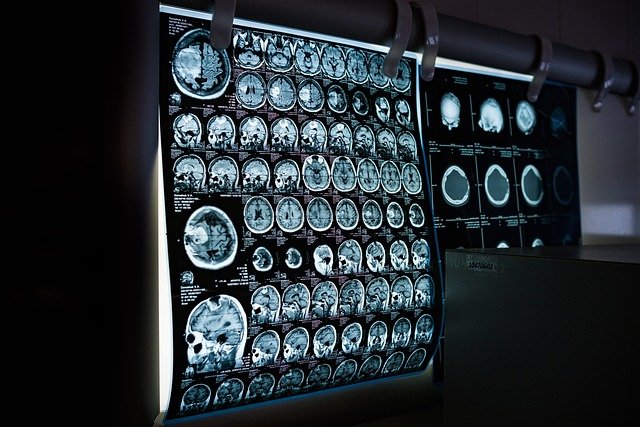
Sensory impairments affecting hearing and vision represent common clinical presentations across diverse patient populations. These disturbances can stem from multiple etiologies, ranging from benign age-related changes to more complex neurological conditions. Medical professionals emphasize the importance of comprehensive evaluation when patients present with unexplained sensory deficits, particularly when symptoms develop rapidly or occur alongside other neurological signs.
The human sensory system relies on intricate neural pathways connecting sensory organs to processing centers within the brain. Disruptions along these pathways can manifest as hearing difficulties, visual field defects, or distorted sensory perception. Clinical assessment typically involves detailed patient history, physical examination, and diagnostic imaging to identify underlying causes and guide appropriate treatment strategies.
How to Detect Neurological Conditions Early: Key Signs
Early recognition of neurological warning signs remains crucial for timely medical intervention. Patients should monitor for sudden changes in sensory function, including progressive hearing loss affecting one ear, unexplained vision changes, or persistent headaches accompanied by sensory disturbances. Additional concerning symptoms include balance difficulties, coordination problems, unexplained nausea, seizures, or cognitive changes such as memory difficulties or personality alterations.
Neurological conditions affecting sensory function may present gradually or suddenly. Progressive symptoms developing over weeks or months require medical evaluation, as do acute changes occurring within days. Family members often notice subtle changes before patients themselves recognize significant alterations in sensory perception or cognitive function.
Early Recognition of Neurological Disorders: What You Should Know
Neurological disorders encompass a broad spectrum of conditions affecting the central and peripheral nervous systems. Understanding risk factors helps individuals recognize when heightened vigilance is appropriate. Age represents a significant factor, with certain conditions becoming more prevalent after age 50. Family history of neurological disorders, previous radiation exposure to the head or neck region, and certain genetic syndromes may increase individual risk profiles.
Medical professionals utilize various diagnostic tools to evaluate neurological function. Audiological testing assesses hearing function and identifies patterns suggesting neural involvement. Ophthalmological examinations, including visual field testing and fundoscopic evaluation, detect vision abnormalities. Advanced imaging techniques such as magnetic resonance imaging (MRI) and computed tomography (CT) scans provide detailed visualization of brain structures, enabling identification of anatomical abnormalities.
Recognizing Neurological Symptoms Early: Signs, Risks, and Medical Advice
Clinical presentation of neurological conditions varies considerably based on location and size of affected areas. Sensory symptoms may include unilateral hearing loss, tinnitus (ringing in ears), double vision, visual field defects, or progressive vision deterioration. Motor symptoms such as facial weakness, difficulty swallowing, or limb weakness may accompany sensory changes. Cognitive symptoms including confusion, memory problems, or difficulty concentrating warrant prompt medical attention.
Healthcare providers recommend seeking immediate evaluation for sudden severe headaches, particularly those described as the worst headache ever experienced, sudden vision loss, acute hearing loss, seizures, or focal neurological deficits. Less acute symptoms developing gradually still require medical assessment, though urgency may be lower. Documentation of symptom progression, including timing, severity, and associated factors, assists healthcare providers in diagnostic evaluation.
Understanding Diagnostic Approaches and Medical Evaluation
Comprehensive neurological evaluation begins with detailed medical history and physical examination. Neurologists assess cranial nerve function, motor strength, sensory perception, reflexes, coordination, and cognitive function. Specialized testing may include audiometry for hearing assessment, visual field testing, and balance evaluation.
Imaging studies provide critical diagnostic information. MRI scans offer superior soft tissue visualization, making them preferred for detailed brain evaluation. CT scans provide rapid assessment and excel at detecting certain abnormalities. Additional testing may include electroencephalography (EEG) for seizure evaluation, lumbar puncture for cerebrospinal fluid analysis, or biopsy procedures when tissue diagnosis is necessary.
Treatment Options and Management Strategies
Treatment approaches depend on specific diagnosis, location, size, and individual patient factors. Management strategies may include observation with regular monitoring, surgical intervention, radiation therapy, chemotherapy, or combination approaches. Supportive care addresses symptoms such as pain, nausea, or seizures, improving quality of life throughout treatment.
Rehabilitation services play important roles in managing sensory deficits. Audiological rehabilitation assists patients with hearing loss through hearing aids, assistive devices, or communication strategies. Vision rehabilitation helps individuals adapt to visual impairments through adaptive techniques and assistive technology. Physical therapy, occupational therapy, and speech therapy address motor and communication difficulties.
Prognosis and Long-Term Considerations
Outcomes vary significantly based on specific diagnosis, stage at detection, treatment response, and individual patient characteristics. Early detection generally correlates with improved treatment options and outcomes. Regular follow-up care monitors treatment response, detects recurrence, and manages long-term effects.
Patients benefit from multidisciplinary care teams including neurologists, neurosurgeons, oncologists, radiologists, and rehabilitation specialists. Psychological support and counseling help patients and families navigate diagnosis, treatment, and adaptation to potential functional changes. Support groups provide valuable peer connections and practical advice from others with similar experiences.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
Maintaining awareness of neurological warning signs empowers individuals to seek timely medical evaluation. While many sensory disturbances result from benign conditions, persistent or progressive symptoms warrant professional assessment. Advances in diagnostic technology and treatment approaches continue improving outcomes for patients with neurological conditions affecting sensory function.




