Exploring System Integration in Healthcare IT Environments
Hospitals, clinics, and municipal services rely on many digital tools to deliver safe, efficient care. When these systems cannot “speak” to each other, work slows and risks increase. This article explains how system integration connects healthcare software and devices, why it matters, and what good integration looks like in practice.
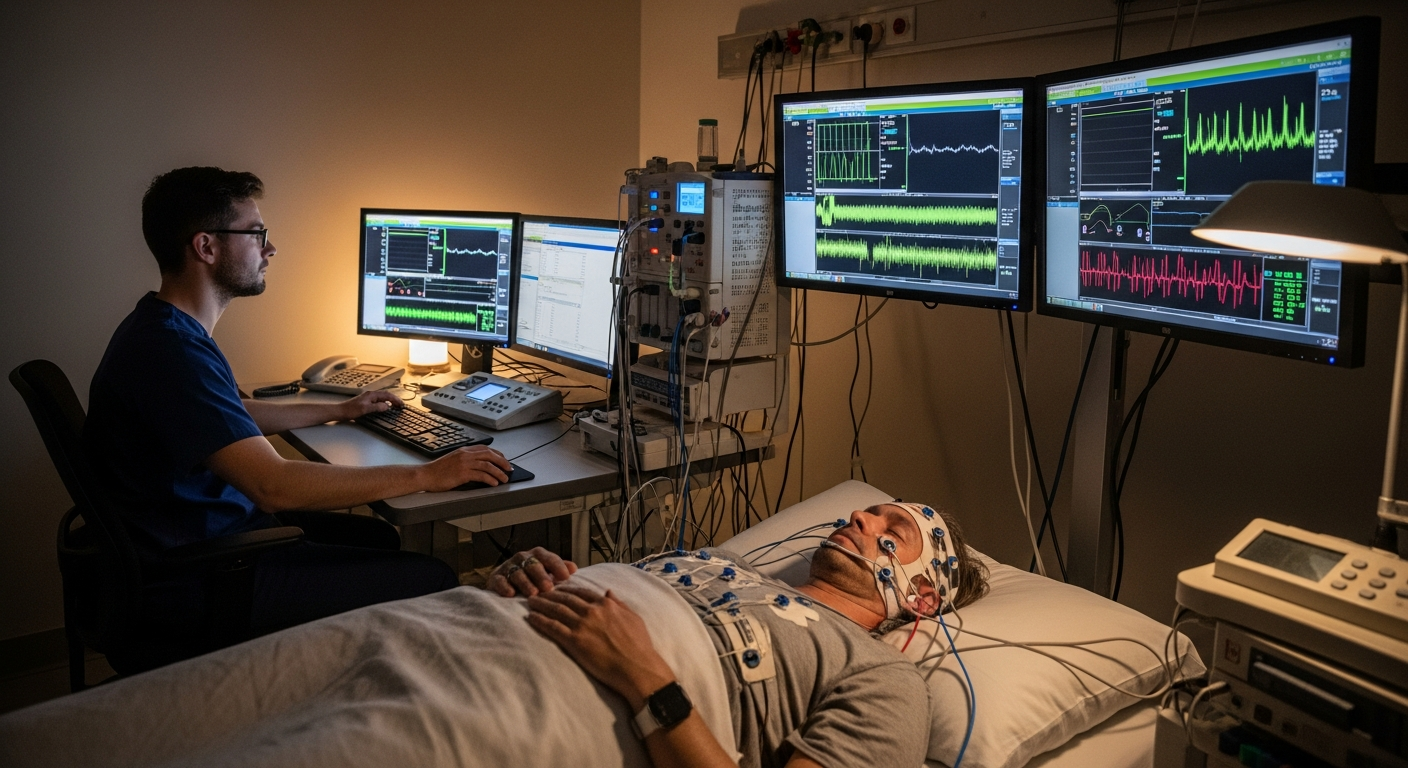
In modern care settings, digital systems handle admissions, clinical documentation, imaging, labs, medications, and billing. Without reliable connections between them, staff duplicate work, information fragments across departments, and decision-making slows. System integration brings these tools together so data flows securely and consistently, supporting clinicians and operations across hospitals, clinics, laboratories, and community services in your area.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
System Integration in Healthcare Information Technology Explained
System integration in healthcare information technology refers to the methods and tools that enable different applications and devices to exchange data accurately and securely. Typical systems include electronic health records (EHR), laboratory information systems (LIS), radiology information systems (RIS), picture archiving and communication systems (PACS), e-prescribing, and medical devices. Integration ensures that a lab result ordered in the EHR appears automatically in the patient chart, that images link to the correct encounter, and that device measurements reach the right record without manual re-entry.
Technically, integration often relies on healthcare standards and interfaces. HL7 v2 remains common for messaging such as admissions, orders, and results. HL7 FHIR supports modern APIs for exchanging resources like patients, observations, and medications. DICOM enables imaging transfer and worklists, while IHE profiles define practical workflows for cross-enterprise document sharing and patient identity management. Integration engines and APIs transform, route, and validate messages so each system receives data in the format it understands, reducing errors and improving reliability.
Understanding the Role of System Integration in Healthcare Information Technology
Effective integration serves clinical quality, safety, and operational efficiency. With unified data, clinicians gain a timely, consolidated view of a patient’s history, allergies, medications, and test results, lowering the risk of incomplete information during diagnosis or treatment. Automated data movement reduces manual transcription, cutting down on delays and transcription errors that can occur when staff switch between systems.
Security and privacy are central. Robust integration enforces role-based access, consent handling, audit logging, and data minimization. Encryption in transit and at rest protects sensitive information, and well-defined interfaces help limit unnecessary data exposure. In European contexts, including Norway through the EEA framework, integration strategies align with GDPR principles by building in purpose limitation, retention controls, and transparency. When systems exchange standardized, high-quality data, analytics also become more trustworthy, informing quality improvement, capacity planning, infection surveillance, and resource management.
Exploring System Integration in Healthcare IT Environments
Designing an integration landscape involves architectural and operational choices. Point-to-point connections are simple for small numbers of systems but become hard to maintain as environments grow. An enterprise service bus (ESB) or an integration engine centralizes routing, transformation, error handling, and monitoring. Event-driven patterns and message brokers support near–real-time updates without overloading clinical applications. Where feasible, FHIR-based APIs provide structured access to resources and can power patient portals, mobile apps, and decision-support services.
Operational excellence is as important as architecture. Version control for interface specifications, automated testing of message mappings, and proactive monitoring reduce downtime. Clear incident response processes help teams resolve failed messages quickly, and dashboarding brings visibility to throughput, latency, and error trends. In your area, collaborating with local services—such as regional health networks, imaging centers, and municipal providers—ensures shared identifiers, consistent coding systems, and agreed workflows across organizational boundaries.
Planning and governance make integration sustainable. Start by documenting the current system inventory, data flows, and known pain points. Define a common data dictionary to harmonize codes and units, and prioritize use cases that reduce clinical risk or administrative burden—such as closing the loop from order to result, or ensuring discharge summaries reach community care. Establish change control so that upgrades to one system trigger impact assessments across interfaces. Finally, invest in training: clinicians and administrative staff benefit from understanding how integrated workflows operate and how to report integration-related issues.
A staged roadmap helps manage complexity. Phase one can stabilize existing interfaces and resolve data-quality issues; phase two can introduce standardized identifiers, terminology services, and FHIR APIs; phase three can expand interoperability with external partners and enable analytics. Throughout, measure outcomes such as reduced duplicate tests, faster result turnaround, fewer documentation gaps, and improved user satisfaction. Even incremental gains—like eliminating a single manual step in a high-volume process—can compound into meaningful time savings across an organization.
Conclusion Well-executed system integration unifies data, streamlines workflows, and strengthens privacy and security across diverse healthcare applications. By combining proven standards with disciplined operations, organizations can reduce errors, accelerate information flow, and support informed decisions at the point of care. In Norway and elsewhere, aligning architecture, governance, and collaboration with local services provides a practical path to resilient, interoperable healthcare IT.




